Medical recordkeeping policy in the pre-Gulf War period was made primarily by the individual military services and contained in their regulations and instructions. These written policies focused largely on the health care of garrisoned (non-deployed) servicemembers in peacetime and said comparatively little about recordkeeping under deployment conditions. Full individual health records were to accompany military personnel on deployment, although this policy would be reconsidered and reversed by the Army and the Air Force. Guidance on the documentation of routine immunizations was detailed, but did not appear to anticipate the use of investigational vaccines or the need for operational security—issues which would arise during the Gulf War and which continue to be of concern to both veterans and policy makers today.
While general guidance for recordkeeping is provided by the Department of Defense, specific medical recordkeeping policies in place at the start of the Gulf War were largely contained in the services’ regulations and instructions.[2] Army and Air Force regulations applied to both active duty personnel and their respective reserve and national guard components. Navy instructions applied also to the Marine Corps, and to the Navy and Marine Corps reserve components.
Content of the record: The individual health records (outpatient records) maintained by the military services were similar in content, although the terms used to describe these records, and the corresponding inpatient records, were different (Table 1).
Table 1. Pre-Gulf War medical record terminology
| MILITARY SERVICE | INDIVIDUAL HEALTH RECORD (outpatient record) | HOSPITALIZATION RECORD (inpatient record) |
| Army | Health Record (HREC) | Inpatient Treatment Record (ITR) |
| Navy (and Marine Corps) | Military Health (Medical) Treatment Record | Inpatient (Clinical) Treatment Record |
| Air Force | Outpatient Record | Inpatient Record |
Medical information included in these records was generally written on Standard Forms (SF), Department of Defense (DD) forms, and service-specific forms and held in a two-part record jacket. The content of particular importance for deployment recordkeeping included the documentation of clinical care (SF 600), clinical consultations (SF 513), immunizations (SF 601), eyewear prescriptions (DD 771), summaries of inpatient care (SF 502), and physical profiles (service-specific forms). (See Tab C for selected medical record forms cited in this paper.)
Although not specifically addressed in medical recordkeeping policy, information from the individual health record would likely be reviewed at the time of mobilization for deployment to ensure the medical "deployability" of the servicemember. Full individual health records were then to accompany all servicemembers on deployment. The Army provided more specific instruction on the maintenance of health records under combat conditions. Individual health records were to accompany servicemembers on deployment and remain in the custody of the appropriate personnel officer. Newly-generated medical information was to be added directly to the health records.[3] Individual health records were to accompany Air Force servicemembers also, but only if the deployment was expected to last 30 days or longer.[4]
The policy on documentation of immunizations received by servicemembers deserves special mention. In the pre-Gulf War period this guidance appeared both in the service regulations and instructions mentioned above, and in a specific instruction, Immunizations and Chemoprophylaxis. An Immunization Record (SF 601) was to be prepared for each member of the Army, Navy, and Marine Corps and maintained in the individual health record. (This form was generally not used by the Air Force.) The instruction also required documentation of immunizations on the International Certificates of Vaccination (PHS 731), commonly called the "yellow shot record." This pocket-sized record was to be prepared for all servicemembers and to serve as the official record of immunizations received for international travel.[5]
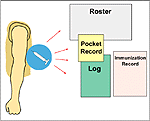
Whether this record was to be carried by servicemembers or remain in their individual health records at other times (especially during deployments) varied among the services and components. Army active duty and reserve personnel were instructed to keep it in their custody. Army National Guard personnel would be issued the record upon mobilization or activation, but Army National Guard units had the option to retain this record in the individual health records. For active duty and reserve Navy and Marine Corps personnel, the International Certificates of Vaccination was to be filed on top of the Immunization Record (SF 601) in the health record, given to the servicemember for travel or mobilization, and returned to the health record upon completion of travel or mobilization. Air Force guidance did not specifically comment on the custody of the International Certificates of Vaccination.[6] Figure 3 illustrates these and other records that may contain information about immunizations.
Figure 3. Records containing immunization information (pre-Gulf War)
Service regulations and instructions did not provide or make reference to any specific guidance for the recordkeeping that might be required for investigational drug and vaccine use under deployment conditions, or for drugs (like pyridostigmine bromide and ciprofloxacin) distributed widely to servicemembers under the same conditions.
Consolidation of the record: Service regulations and instructions indicated the need to consolidate medical information generated by different providers and in different facilities for inclusion in the individual health record. While records of hospitalizations have always remained separate and distinct from the individual health record, summaries of this inpatient care were to be forwarded to and included in the individual health record.[7]
Specific guidance on the generation and handling of immunization rosters and logs was not included in these medical recordkeeping regulations and instructions, perhaps because these records often originate from personnel offices. Yet the expectation that this information would be annotated in the individual health records can be inferred from the detailed instructions on maintaining immunization records, as noted under the Content of the record section above.
All services had elaborate yet service-specific guidance on the handling of stray treatment forms. If enough identifying information was available, extensive efforts were to be made to locate the individual health record and forward the stray forms for inclusion. If identifying information was missing or insufficient, the forms could be destroyed following a review by a medical facility committee.[8]
Custody of the record: While individual health records and hospitalization records (inpatient records) are the property of the US Government, all services had established procedures to allow access to these records by servicemembers, and by medical providers and others who had a legitimate need to see this information. The need to maintain the confidentiality and security of medical information was suitably emphasized in pre-Gulf War regulations and instructions.
For garrisoned servicemembers, individual health records were ordinarily to be retained and maintained in a designated military medical facility. When servicemembers changed duty stations, their health records were also to be transferred, often hand-carried by the servicemembers themselves.[9] Upon servicemembers’ separation or retirement, individual health records were to be combined with personnel records by the services and forwarded to the National Personnel Records Center (NPRC) in St. Louis, Missouri for permanent storage.[10] (The NPRC is a records storage facility of the National Archives and Records Administration or NARA.)
Hospitalization records were to be handled differently. These records were to be retained by the medical treatment facility at which the servicemember was hospitalized, then eventually forwarded to the NPRC.[11] Inpatient records were not to be combined (for storage) with the individual health records, but were to be stored at the NPRC in separate groups according to the year and medical facility in which hospitalization occurred.
The unique and unanticipated requirements of the Gulf War led to revisions of medical recordkeeping policy. Of special importance were the deployment of an abstract of the individual health record in place of the record itself, and the sometimes vague and conflicting attempts to meet the need for documentation of immunizations which were investigational or required operational security. These policies generated questions over where, and even whether, to document this immunization information. Contradictory or confusing policy may also have been a factor in determining what and how medical documents would be retained, and where they would be located after the war.
The services provided additional recordkeeping guidance during the pre-deployment, deployment, and post-deployment phases of the Gulf War. Consistent with the operational organization of the military, the command for Southwest Asia (US Central Command or CENTCOM) also played a major role in establishing elements of this guidance. Policy additions and changes during this period were largely contained in memoranda and messages. These statements modified the documentation requirements for some immunizations and, for some services, directed the deployment of an abstract of the individual medical record rather than the record itself. These changes in policy may have had some bearing on the completeness and availability of medical records from this period.
Content of the record: During the initial phase of deployment, Army and Air Force policy statements directed that one-page health forms, prepared at the time of mobilization, accompany servicemembers in place of individual health records. This change was very likely influenced by the aircraft crash in 1985 at Gander, Newfoundland, in which 236 members of the 101st Airborne Division perished, along with their medical records.[12] The Navy and Marine Corps, however, continued their policies of deploying personnel with full individual health records.
… personnel from her unit were told their original medical records would not be taken to the Gulf [from home station].… new records would be issued to them once they arrived.… those records [Gulf War records] are now lost. -related by an aeromedical evacuation technician[13]
For the Army this was an interim step in an effort begun several years earlier to eliminate paper records from the battlefield, and eventually to store health, personnel, and finance information on an electronic device, the Individual Carried Record (ICR), later the Personal Information Carrier (PIC). Upon mobilization, health care information essential for deployment was to be abstracted from the individual health record and written on a one-page Individual Medical History form (IMH) (HSC 621-R-Test), also called the Medical Readiness Form (MRF), and later the Individual Medical History form (DA 8007). The completed form was then to accompany the soldier on deployment as the basis of a medical field file, and to be retained by the medical treatment facility responsible for the health care of the soldier. Any health information generated during the deployment would be added to this field file.[14] While direction to prepare and deploy the Medical Readiness Form was included in written policy prior to the Gulf War,[15] it appears that full implementation of this form did not occur during the large-scale mobilization effort.
In January 1991, the Air Force also changed its earlier policy of deploying personnel with their individual health record (see section III.A. Pre-Gulf War Policy), and substituted for this record the one-page Summary of Care form (AF 1480). (This change was driven by deep concern from operational headquarters that medical records might be lost or destroyed, and that the risk of loss outweighed the possible medical benefits of having the complete record.[16]) The AF 1480 form was to be completed from information in the individual health record at the time of pre-deployment screening, and was to accompany Air Force personnel on deployment. For individual health records already in theater, AF 1480 forms were to be completed as time permitted, and the individual medical records returned to home bases.[17] The Air National Guard issued similar policy stopping the deployment of individual health records.[18]
She recalls asking if the [anthrax] shot was to be entered in their medical records and was told not to since it would be recorded by computer. She entered it into individual medical records anyway. -related by a hospital corpsman[19]
The guidance on documentation of immunizations was complicated by the need for operational security in the use of the anti-biological warfare anthrax and botulinum toxoid vaccines, and by the documentation requirements for the investigational botulinum toxoid vaccine. The investigational new drug protocol submitted by the DoD to the Food and Drug Administration (FDA) for use of this vaccine stated that receipt of each vaccine dose would be recorded "in the individual’s permanent vaccine file," and that attempts would be made to maintain a roster including name, social security number, date, and the unit of all individuals receiving each vaccine dose.[20]
In January 1991, CENTCOM and Army messages, originally classified SECRET and since declassified, provided guidelines for the theater-wide anthrax and botulinum toxoid vaccination programs. Both messages cautioned recipients of these vaccines not to discuss them with anyone, then stated that the vaccinations may be recorded on the yellow shot record (PHS 731), or on the Immunization Record (SF 601), as Vacc A and Vacc A-2 (for the anthrax series) and Vacc B, Vacc B-2, and Vacc B-3 (for the botulinum toxoid series).[21] (A later memorandum indicated these vaccines may also have been recorded as "Anthrax," "A Vaccination," "A-Vax," "Botulinum," "Bot-Tox," "B Vaccination," "B-Vax," or something similar.[22] )
For anthrax vaccine, it appears that a roster of personnel receiving the vaccine was required. For botulinum toxoid vaccine, personnel were required to sign an information sheet about the vaccine, indicating that they had read and understood the information and had voluntarily submitted to this immunization.[23] (See Tab C.) The information sheet appears to have been designed to hold 22-25 entries per sheet and to serve perhaps as a roster of vaccine recipients as well as a "consent form" for this investigational vaccine. (Several days before the CENTCOM message cited above, the FDA had granted the DoD a waiver from the requirement to obtain informed consent from personnel receiving the botulinum toxoid vaccine. Nonetheless, it appears that CENTCOM ultimately decided to administer the vaccine on a voluntary basis.[24] ) No specific guidelines for the maintenance or forwarding of these records (rosters and information sheets) were included in these early messages.
… told them not to document any vaccines and new medications in the Marines’ records. They did rosters when the shots were done but no units were noted on them, so there was no way to go back and enter the data later. -related by a hospital corpsman[25]
Whatever the initial guidance, there appeared to be substantial confusion in the months that followed about where, even whether, these vaccinations were to be recorded. From March to July 1991, messages and memoranda from the Army, Army Reserve, National Guard Bureau, and Marine Corps appeared to rescind the earlier instructions not to record, and to require that a record of the vaccinations be entered in the individual health records and that rosters of immunized personnel be forwarded. These documents directed Army units to forward their rosters through the chain of command to the Office of the Surgeon General, and First Marine Division units to send their rosters and information sheets to the First Marine Expeditionary Force Surgeon’s Office.[26]
[Vaccinations were] posted on shot records, and list of names checked off [a roster]. -interview with a clearing company physician[27]
Medical recordkeeping policy provided little specific guidance for the documentation of drugs distrbuted widely to servicemembers as preventive measures against biological and chemical agents. Drugs such as ciprofloxacin (for anthrax) and pyridostigmine bromide (for a nerve agent) are normally distributed to servicemembers, then self-administered under the direction of operational commanders. These circumstances present challenges for documenting the use of such drugs in either individual health records or unit records. Pyridostigmine bromide, like botulinum toxoid vaccine, was also an investigational product during the Gulf War. The FDA, under a newly enacted interim rule, had granted a waiver from the requirement to obtain informed consent from servicemembers taking this drug, but this rule did not address the recordkeeping that would ordinarily accompany the use of an investigational drug.[28]
Consolidation of the record: The Army provided specific guidance for connecting the field file (containing the abbreviated health record and medical information generated during deployment) with the permanent individual health record at the time of demobilization. This consolidation was to occur at the facility usually responsible for maintaining the record, ordinarily the Army Personnel Center, the National Guard Bureau, or for those remaining on active duty, the medical treatment facility of their home station.[29] Although not specifically stated in the Air Force policy modifications, abbreviated health records, along with any additional medical information generated during deployment, would likely be returned for consolidation with the individual health records at the time of re-deployment. Guidance on an abbreviated health record for Navy and Marine Corps personnel was not necessary, since those servicemembers deployed with their full individual health records.
The plan was to send copies of treatment records home. Most of the time this never happened.… she was treated in-country and none of the treatment records ever made it home. -interview with an aeromedical technician[30]
Assuming most Army units in the Gulf deployed without individual health records and recognizing the need for deployment-specific guidance, the XVIII Airborne Corps recommended to the Army Central Command a series of procedures for dealing with the largely outpatient health record forms generated in theater. Health record forms generated at battalion aid stations and divisional clearing stations (normally for servicemembers attached to these units) would either be maintained there for the duration of deployment or sent periodically to the installation from which the soldier departed. This latter route was emphasized for health record forms generated at corps level medical detachments and at clearing companies and platoons. For units that deployed with individual health records, in-theater forms would be consolidated with these records.[31] A response from Army Central Command regarding these recommendations could not be located.
The Army also saw the need to simplify medical recordkeeping for in-theater hospitalizations, and in November 1990 issued an exception to the policy for the use of the Abbreviated Medical Record form (SF 539). This form, designed as an abbreviated inpatient record for hospitalizations of less than 72 hours, was authorized for use as the record of hospitalizations that exceed that time limit, provided they were uncomplicated. For complicated hospitalizations this exception did not apply, and a summary of the inpatient care (SF 502) needed to be completed (and presumably a copy included in the individual health record).[32] Pre-Gulf War Army guidance did not specifically include the SF 539 form as part of the individual health record, although there is a mention to include "other SF 500 series forms."[33] Navy guidance specifically listed SF 539 as part of the individual health record; Air Force guidance mentioned only "other SF forms."[34]
After the War, patient records [originals and duplicates] were boxed up and sent to St. Louis for storage.… there was confusion as to where these records were to be sent and stored. He chose St. Louis in his best judgement, but the receiving organization refused to receive the records… [the hospital] was not on their list of recognized commands…. they eventually were sent to [a stateside hospital] for storage. -interview with a hospital commander[35]
Custody of the record: As was the policy before the Gulf War, inpatient records were ordinarily to remain in the medical treatment facility where the hospitalization occurred, with a summary of this hospitalization forwarded to the individual health record. In November 1990, the Air Force re-emphasized this policy to its in-theater hospitals, directing that the inpatient records be retained by the hospitals for the duration of the deployment, then returned to the home station with the unit at the end of the deployment.[36] Air Force policy for its European contingency hospitals, however, allowed the inpatient record to accompany a patient transferred for further medical care; otherwise, the original record was to be maintained by the contingency hospital and brought back to the continental United States when the facility closed.[37] In December 1990, the Army’s XVIII Airborne Corps recommended to the Army Central Command a continuation of existing policy that inpatient records initiated at deployed hospitals would either accompany patients transferred to other treatment facilities, or be retained at the deployed hospitals and retired (sent to the National Personnel Records Center) at monthly intervals.[38] As noted previously, a response from the Army Central Command to this recommendation could not be located.
During the Gulf War, the Army and the Air Force also provided modifications to their general recordkeeping policies that apparently applied to all Gulf War records. These policy statements did not always specifically mention or exclude individual medical records, inpatient records, and other health-related documents. In February 1991, the Army established procedures for the retirement of Desert Storm records as an exception to its earlier established regulation. Records were to be sent to the unit’s home station, if the unit had a home station, or, if it did not, to the US Army Information Systems Command (USAISC-Pentagon) for appropriate action. Although the guidance in this memorandum did not differentiate between medical and non-medical Desert Storm records, an enclosure provided specific instructions for medical records. Army outpatient field files were to be returned to the home or mobilization station and combined with the individual health records. Inpatient records (except for those transferred with patients to other medical facilities) were to be forwarded to the USAISC Operation Desert Storm Records Holding Area in Alexandria, Virginia.[39] In January 1991 and in the following months, the Air Force also provided new policy for dealing with Gulf War records. This policy apparently applied to operational rather than medical records, but may have been a source of confusion, since medical records were not specifically mentioned.[40]
| First Page | Prev Page | Next Page |